Breaking the silence: A man’s experience with breast cancer
Rod Ritchie’s personal journey in the uncharted territory of male breast cancer
- 02/23/24

Breast cancer is a rare diagnosis for a male, and my experience shows how its rarity can lead to a late diagnosis, which is a common result.
In 1962 my mother died of metastatic breast cancer, leaving behind a devastated husband and three young kids. I was 12. Fast forward 62 years, and I’m feeling a lump behind my left nipple. My first thoughts weren’t breast cancer. I thought I likely had a cyst, which is common. At my next general physician’s appointment, I mentioned the lump as an aside to a few other concerns, including hypertension. She didn’t perform a clinical examination but convinced me to wait and see whether the lump would disappear in time. A watch-and-wait exercise.
A month later, there was no improvement. I returned to my doctor and got the same “treatment” and the same advice. Finally, three months after the first visit, I had an inflamed breast and inverted nipple. I confronted my GP. I pointed out that my mom’s death was on my medical record, and at that moment, my GP and I suddenly suspected there was a potential tumor to be found. Sure enough, two days later, the sonographer looked worried as she glided a transducer over my chest. When she disappeared to fetch a senior doctor, I was getting the message loud and clear.
Facing the diagnosis: Stage IIIB inflammatory breast cancer
Three days later, a fine-needle biopsy showed Stage IIIB inflammatory breast cancer. This was March 2014. I went to see a breast surgeon who took one look at my breast and referred me to a medical oncologist. From her I learned that my treatment plan included neoadjuvant (pre-surgery) treatment to eliminate the inflammation and shrink the tumor; then surgery would be possible. This is the standard course of treatment for inflammatory breast cancer. On the way out the door, the doctor asked, “Do you have a family history of cancer?” Well, since you asked, yes. Subsequent genetic testing revealed a BRCA1 mutation but with a variant of uncertain significance (VUS).
Tolerating the unknown: Beginning treatment
I was worried about chemotherapy: What if I couldn’t tolerate it? After expressing my concerns, my oncologist gave me one of the best bits of advice I have received to date. She said, “Don’t have any preconceived notions about any stage of treatment.” This sounded so logical. As it turned out, the 18 weeks of chemotherapy, three lots of FEC (fluorouracil, Ellence, and Cytoxan, and three of docetaxol), went very well for me, and I tolerated the drugs without many of the usual side effects.
After a break of a few weeks, it was back to the breast surgeon for a mastectomy. People asked me, “What? How can you have one of these?” Well, I’d explain, all sexes have breast tissue, but breasts develops further in women following puberty. So, yes, as my small amount of breast tissue was quite badly off, it required extensive surgery, along with removing all of the axillary lymph nodes in my left arm. With 2/23 lymph nodes having cancer, this meant a risk for local recurrence. For some reason reconstruction was not on the agenda. Was this because I was a man, and who would care if there was a scar on one side of my chest? No, my breast surgeon explained, because the surgery was extensive, there was not enough remaining extra material to rebuild the breast. In any case, this was a low priority for me, and I was not going to insist on having a plastic surgeon do their best. I just thought, one operation is enough.
Post-mastectomy realities: Challenges and hopes
At the post-surgery meeting, I learned that, unfortunately, pathological complete response (pCR) had not been achieved—the treatment so far had not gotten rid of all the cancer. I was booked for 33 daily doses of radiation once the scars had healed and the last of the seromas drained. Recommended as “insurance,” the rads, as they are sometimes called here in Australia, were to zap any remaining cancer cells in my skin, the chest cavity, and under my left arm where all my lymph nodes were removed.
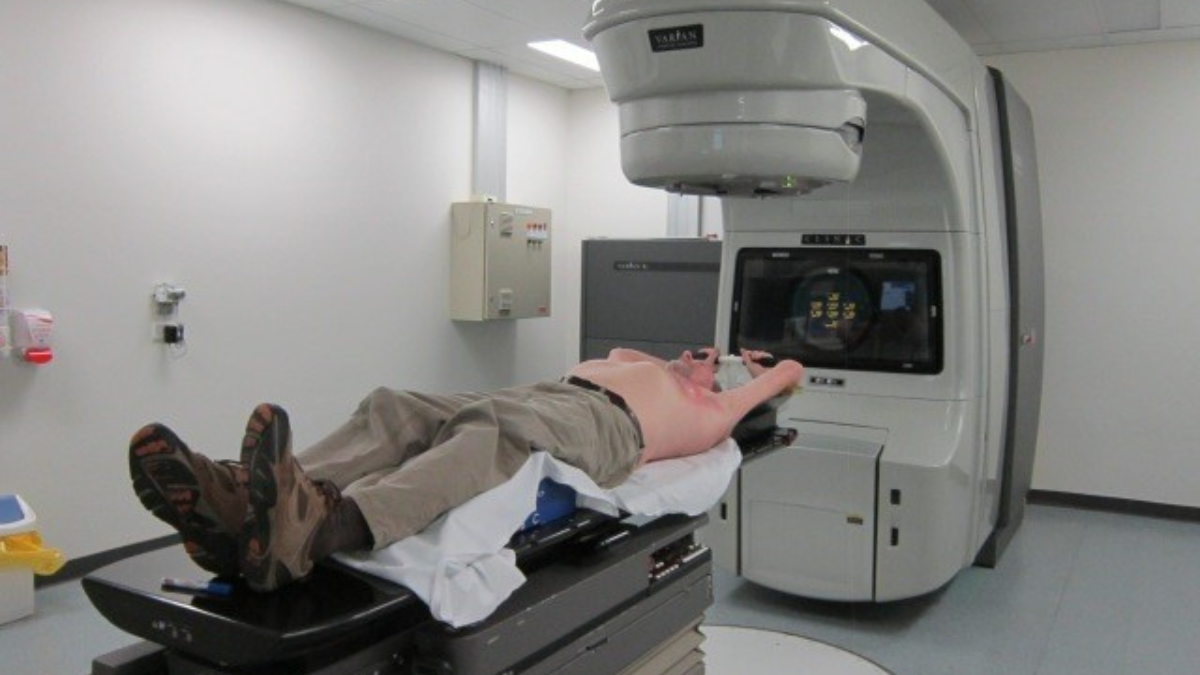
Radiation, the final treatment: Am I cured?
This seemed like a dumb question, but I asked it anyway. My tolerant oncologist said, “No, not until all cells in your body are free of cancer.”
“Oh,” I thought, “that’s not good.”
She quickly added, “Look, we’ve prescribed what I might call the ‘kitchen sink’ treatment. You had the works, and now I’m going to put you on the hormone blocker tamoxifen.”
“Oh,” was my retort, “the drug that gives you hot flashes?”
“Hopefully not,” she replied, “since you’re an older guy.”
Apparently younger men can suffer from this.
All this was eight years ago.
Two years after my breast cancer diagnosis, I was diagnosed with an aggressive prostate cancer and treated solely with surgery, a radical prostatectomy. Yes, a second primary cancer. For some reason, I’ve put this cancer, one of the most diagnosed of all male cancers, in the back of my mind because it didn’t need nearly as much treatment as the breast cancer, and because it was, I later learned, not uncommon for men with a breast cancer diagnosis to get prostate cancer. And, I should note, vice versa.
Breaking the stigma: Advocacy for gender-neutral cancer awareness
Certainly, as a writer, there’s more to go on about as a guy with breast cancer. I quickly learned that men in my position were comfortable dealing with prostate cancer, but overly stigmatised learning they had breast cancer. “Oh, a woman’s disease” was the most common comment. This was my “aha” moment. I knew I needed to advocate for this issue.
Most fortunately, I’m currently NED (no evidence of disease) for both cancers.
I was so fortunate my late diagnosis didn’t lead to me being Stage IV de novo, like many of my friends, both women and men. With breast cancer in my family history, I have made my siblings and adult kids breast-aware, so that they know to screen themselves regularly. While I didn’t want to worry people unnecessarily, I didn’t want to underplay the threat to them either. I think it’s unfair that while my late-forties daughter is in a public screening program, my son, not much younger, has to fend for himself.
Apart from a later diagnosis, I can’t complain about any aspect of my treatment and I certainly don’t feel any less fortunate to get this disease than anybody else. All my speciality medical treatment was from top-class female doctors and surgeons. I was lucky to benefit from the skill and experience of healthcare providers trained to treat the number one female cancer. Understandably, since treatment, I have spent much of my time advocating for awareness based on the fact this disease is genderless. And I keep saying men need to cast off what are, very often, perceptions of stigma of a diagnosis and understand: gender matters little when it comes to successful treatment.
This blog was updated on February 23, 2024, for minor changes in the title and to add headers.
Stay connected
Sign up to receive emotional support, medical insight, personal stories, and more, delivered to your inbox weekly.


