Dealing with fears, finding support and inspiration: Jae Troskosky
Jae shares how their family history of cancer, a breast cancer diagnosis, and fears about discrimination sparked an interest in advocacy.
- 03/09/23

At age 31, Jae Troskosky had a plate of responsibilities that was especially full. Since graduating college, Jae had been caregiver to their ailing mother and father, while also working full-time as a teacher in a child care center.
By early 2021, Jae’s mother, who had endured pneumonia and a heart attack, was hospitalized with congestive heart failure. The following month, Jae’s father was hospitalized for uncontrolled high blood pressure.
In April, Jae noticed a breast lump and went to their primary care doctor. The doctor said the lump felt benign but it should be checked out. Jae agreed to do that. “And then my mother passes away,” Jae says. “At that point, I decide we’re going to put everything on hold until I get her affairs in order.”
Soon, Jae was hospitalized with a ruptured ovarian cyst, caused by polycystic ovary syndrome (PCOS) diagnosed when Jae was 26. Surgery and recovery further delayed getting the breast lump checked out. Then their father was in a car accident.
In late December, Jae went for a mammogram. They learned the lump was breast cancer on January 7, the Greek Christmas, which Jae’s family celebrates. “Well, Merry Christmas to me!” Jae says ruefully, recalling that moment. “It felt like somebody decided to take a baseball bat and hit me over and over with it.”
Jae was diagnosed with stage III breast cancer. Treatment would start with chemotherapy, followed by bilateral mastectomy, radiation therapy, and hormonal therapy. It was a lot to worry about.
As a nonbinary person, Jae feared encountering discrimination, poor care, and a lack of support from medical providers and others, as some in the LGBTQ+ community have experienced. Having lost several family members to cancer, Jae also struggled with recurrent fears about their own mortality. And there were challenges in continuing to work through treatment and take care of their dad.
One by one, Jae found ways to deal with those fears, find support and inspiration, and even begin a new interest in breast cancer advocacy. Two years after diagnosis, Jae talked with LBBC contributing writer Robin Warshaw about the road that led them to a stronger place.
Robin: Did you start out worried about how your medical team would react to you being a non-binary person?
Jae: Oh, absolutely. I had friends who did not receive the same level of care because they were part of the LGBTQ+ community. And there’s been people throughout my life, friends who received some discrimination because they were part of the LGBTQ+ community. So it was an honest fear that I wasn’t going to receive the same level of care.
A lot of people are afraid to be open with their medical team about their sexualities or about their gender identities.
I’m very open about this. I am a nonbinary, agender person. I’m asexual.
Robin: How did your medical experience match up to your fear of being discriminated against?
Jae: I was lucky, because my team was amazing. There was no judgment from them. I was very pleasantly surprised.
When I told my surgeon that I wanted to do the double mastectomy with no reconstruction in order to fit my gender-neutral identity, he said, “Oh, yeah, that’s fine. I support it.” And my primary care team was supportive about it.
The week before I was going for radiation, I got a phone call saying, “Hey, we see in the notes that you identify as gender neutral. Which changing room would you like to use?” That was the first time anyone ever asked me that. I thought, “Wow, this is supportive.”

I had friends who did not receive the same level of care because they were part of the LGBTQ+ community. So it was an honest fear that I wasn't going to receive the same level of care.
Robin: Did others push back against your decision to go flat?
Jae: The thing is, gender does not define me.
My father said, “I’m really happy that you’re not all upset about losing your breasts.” I said to him, “It’s because my value as a person doesn’t depend on me having breasts or having a feminine physique. I know my value as a person is who I am and what I do for others.”
I am a teacher. I’m an artist. I create and play music, and I read. That is who I am.
Robin: How did having a family cancer history affect you?
Jae: My grandmother passed away with colon cancer, my uncle passed away of throat cancer. My cousin had stage I breast cancer. I got this cancer diagnosis and I’m immediately thinking, “Am I next?”
I was terrified, fully despairing. The phrase, “How much time do you really have left?” kept repeating in my head even on the best of days.
I did a drawing that was like the thoughts in my head. There was a skull and a lily and a melting clock. There were other artworks where I would write repeatedly, “How much time do you really have left?”
Eventually everything came to a head. On my first or second day of radiation treatment, I broke down crying in the middle of being seen by one of the nurses. They called in a social worker to help me talk through it because everything had been building up.
Robin: Were you able to use your art to help you?
Jae: I was able to do some art. When I was in chemo or some other treatment, I wasn’t in the right mind to actually do anything. I did art after I got home or when I had the strength to do it, usually on the weekends. I like doing illustrations.
I would get fatigued easily. Mostly I read a lot. I get books from the library and subscribe to some online novel sites.
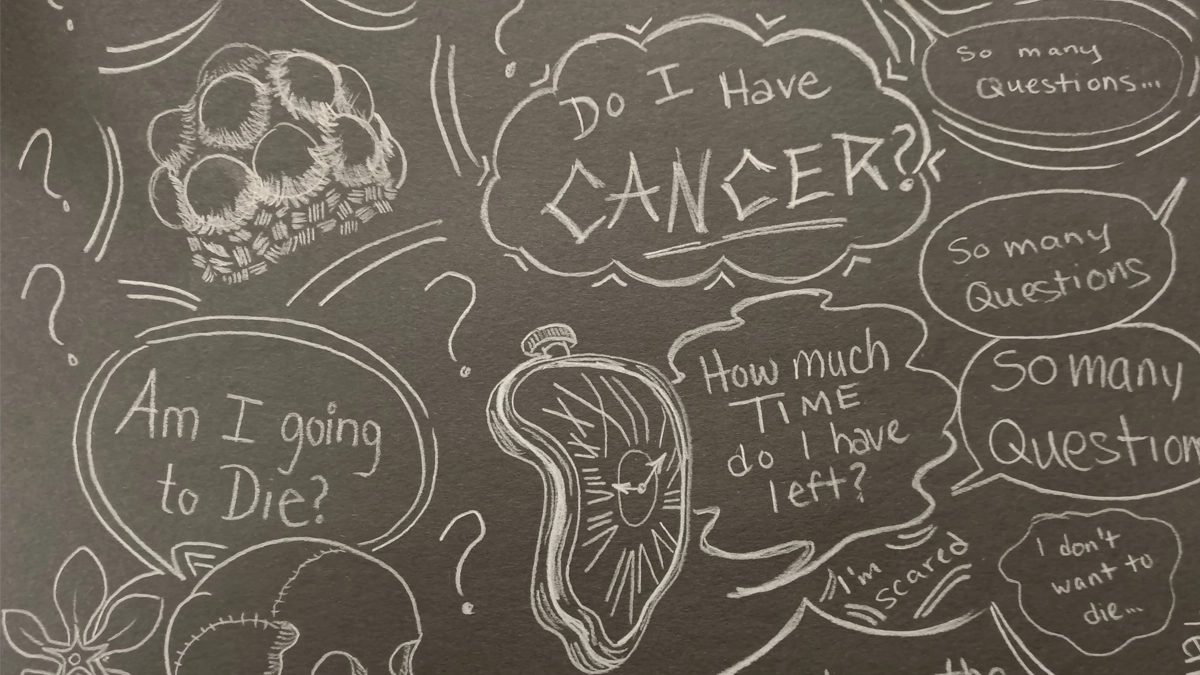
Robin: Did you seek out resources for support? Was there help you wish you had received?
Jae: Because of my family cancer history, I subscribed to the FORCE newsletter. I heard about LBBC through the oncology social worker. When I was considering having reconstruction because society would demand it of me, I saw an LBBC blog by a woman who decided to stay flat after surgery. That helped me cement the decision to go flat.
I wish I could have talked to more people about the diagnosis, especially people who were LGBTQ+. My friend has a girlfriend with MS and I talked with her about having a diagnosis that could change your life. But there wasn’t any real connection to anybody who is LGBTQ+ with cancer.
Robin: You became an LBBC Young Advocate in late 2022. What type of advocacy work would you like to do?
Jae: Through my oncologist’s office, I hope to talk to people to help them understand their diagnosis and that having cancer isn’t necessarily a death sentence.
I can do illustrations to tell the stories of different people from around the country. Some in my Young Advocate group are willing to share their stories and I would illustrate them.
Robin: Have you done any advocacy work already?
Jae: I was on a Zoom panel for the FDA, about the difficulties people of minority groups experience when they get a cancer diagnosis. I was the LGBTQ+ representative. There were at least 55 people in the room.
I explained how while I had a good experience with my medical team, there are fears of disparity of treatment. You don’t think anyone’s going to be discriminated against like that, until somebody tells you, yeah, this happened. At that point, you have to face a new reality.
I’m also going to distribute LBBC material at an International Women’s Day event.
Robin: Why do you want to reach out to others in these ways?
Jae: I’m fairly certain I could have been diagnosed earlier than stage III if I would have just gotten checked out.
I want to help people with breast cancer understand you can’t help others if all you have are the burning embers of who you used to be. You can’t use ashes to light a candle.
It’s vital for people to remember that they have to take care of themselves.
DISCLAIMER:
The views and opinions of our bloggers represent the views and opinions of the bloggers alone and not those of Living Beyond Breast Cancer. Also understand that Living Beyond Breast Cancer does not medically review any information or content contained on, or distributed through, its blog and therefore does not endorse the accuracy or reliability of any such information or content. Through our blog, we merely seek to give individuals creative freedom to tell their stories. It is not a substitute for professional counseling or medical advice.
This article was supported by the Grant or Cooperative Agreement Number 1 U58DP006672, funded by the Centers for Disease Control and Prevention. Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the Centers for Disease Control and Prevention or the Department of Health and Human Services.


