Mammogram
- Medical Review: Kristin Brill, MD, FACS
A mammogram is an imaging test that can detect breast cancer. This imaging approach is known as mammography, and it’s the best technique available to screen for breast cancer and lower the number of deaths from the disease.
If you’ve never had a mammogram, you may have concerns or questions about what the test is, what happens when you get a mammogram, when and how often you should get one, and what the test’s results mean. On this page, we’ll explain the most important things to know about mammograms and provide guidelines from the most trusted organizations.
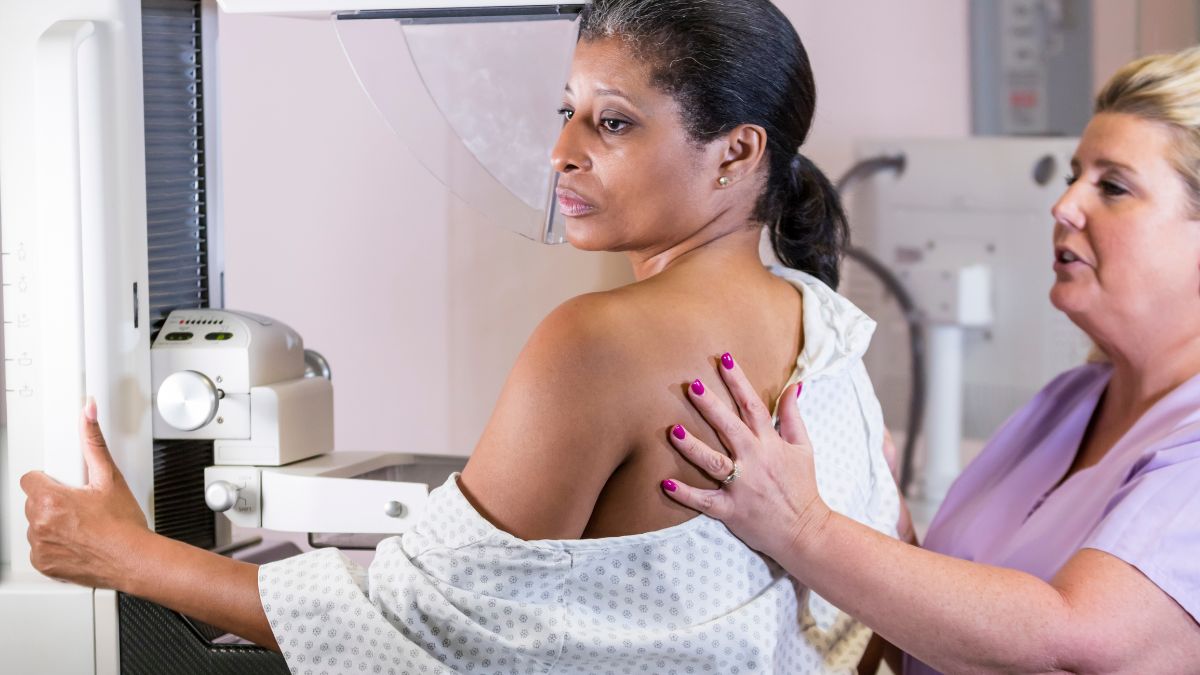
What is a mammogram?
A mammogram is a low-dose x-ray test of the breasts that captures images of breast tissue. The images help doctors to assess breast changes that could be cancer.
Before 2000 or so, mammograms were printed on large sheets of black and white film. Now, digital mammograms are common. Digital mammograms can be recorded and saved as files in a computer. Radiologists can change the contrast of the digital image and zoom in to look more carefully at different parts of the breast.
Screening vs. diagnostic mammograms
You may have heard the terms screening and diagnostic used to describe mammograms. A screening mammogram refers to a mammogram for a person who does not have signs or symptoms of breast cancer.
A diagnostic mammogram is performed if you have signs or symptoms of breast cancer. A diagnostic mammogram may also be used if your doctor needs further study of something seen on a screening mammogram that doesn’t look normal. A diagnostic mammogram may require more pictures of the breast than a screening mammogram.
Who should get a screening mammogram?
Who should get a screening mammogram — and when and how often — depends on certain factors. One of those factors is your sex assigned at birth. Anyone can develop breast cancer, but breast cancer is much more common in women, or people assigned female at birth. Men, or people assigned male at birth, do not undergo regular screening mammograms. Another factor is whether a doctor has recommended you get the test.
Whether you have an average risk or a high risk of developing breast cancer is also an important factor in deciding when you should begin having, and how often you should have, screening mammograms. For screening purposes,
average risk means you:
- Do not have a personal history of breast cancer
- Do not have a strong family history of breast cancer
- Do not have a genetic mutation known to increase breast cancer risk
- Have not had chest radiation therapy before age 30
Mammography screening recommendations
Different professional organizations and groups have different recommendations for mammography in women at average risk. LBBC offers the recommendations of five of these groups here:
| The American Cancer Society (ACS) | National Comprehensive Cancer Network (NCCN) | U.S. Preventive Services Task Force (USPSTF) | American College of Radiology (ACR) | The American Society of Breast Surgeons (ASBrS) | |
|---|---|---|---|---|---|
| Age to start screening mammograms | 45; option to begin at 40 | 40 | 40 | 40 | 40 |
| How often to screen | <54, every year; >55, every other year* | Every year | Every other year | Every year | Every year |
*Every year up to and including age 54; at age 55, option to screen every year or every other year if they are in good health and are expected to live at least 10 more years
For people at average risk, here are the major similarities and differences in mammogram screening recommendations:
- Most of the organizations listed above recommend that screening begin at age 40.
- The exception: The American Cancer Society (ACS) suggests age 40 as an option and 45 as the recommendation.
- Most of the organizations recommend annual screening mammograms (every year), with ACS recommending annual screenings until at least age 54.
- The exception: The U.S. Preventive Services Task Force (USPSTF) recommends screening mammograms every other year.
There are different mammogram screening guidelines for people who are at increased risk of breast cancer. Factors that increase risk include a family history of breast cancer, inherited high-risk genetic mutations such as BRCA1 or BRCA2, and having dense breasts. Learn more about risk factors.
For women who are at increased risk of developing breast cancer:
| ACS | NCCN | USPSTF | ACR | ASBrS | |
|---|---|---|---|---|---|
| Age to start screening mammograms | Between age 30-40* | 30, + breast MRI as early as age 25 | No specific recommendation | 25 or 30* | 30 or 35* |
| How often to screen | Mammogram + breast MRI every year | Mammogram + breast MRI every year | No specific recommendation | Every year** | Every year** |
*Depending on risk factors
**Possibly adding breast MRI, depending on risk factors
Most recommendations for women at high risk for a breast cancer diagnosis include breast MRI as well as mammograms. As shown in the chart above, most of the organizations recommend annual screening mammograms starting between ages 25 and 35 for people at high risk, depending on individual risk factors. The exception is the USPSTF, which does not have specific screening recommendations for people at high risk.
Some states do not legally require health insurance companies to pay for extra screenings for people at high risk. If you are at increased risk of breast cancer and your insurance provider does not cover high-risk screenings, you can learn about options in our Paying for your mammogram section below.
With different professional groups making different and sometimes conflicting recommendations, it can be confusing and frustrating to know what kind of screening plan is best. No matter how old you are, talk with your doctor about your individual risk for breast cancer and what kind of screening plan is most appropriate for you.
Understanding your risk of breast cancer
If you are unsure about whether you are at an increased risk for breast cancer, talk to your doctor about getting a risk assessment. NCCN recommends women have a breast cancer risk assessment by age 25. The ACR recommends women, especially women who are Black or of Ashkenazi Jewish descent, have a risk assessment by age 30. Learn more about risk in Who gets breast cancer?
Two-dimensional (2D) versus three-dimensional (3D) mammograms
You may have heard the terms 2D and 3D mammogram used to describe different kinds of mammograms. Here, we’ll explain what they are and how they are different:
- 2D mammogram: A standard mammogram is two-dimensional, or 2D. With 2D mammograms, x-ray images are taken from two different angles (top to bottom and side to side).
- 3D mammogram: Three-dimensional, or 3D, mammograms take many images as the machine moves in a small arc around the breast. A computer puts these images together, allowing doctors to view the mammography from multiple angles. 3D mammograms are also known as digital tomosynthesis. Many centers offer 3D mammograms, which may allow doctors to see images of breast tissue more clearly.
Some systems automatically apply both 2D and 3D mammography as part of the screening.
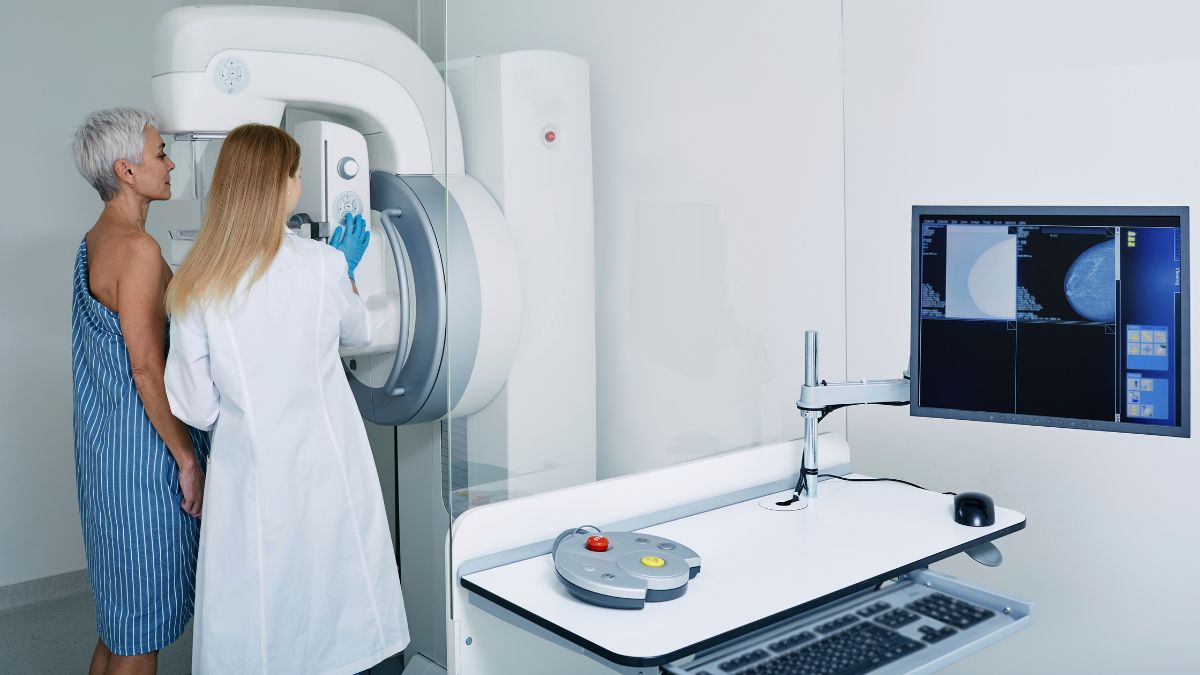
Preparing for your mammogram
There are a few ways to prepare for a mammogram. In this section, we’ll take you through each step.
Scheduling your mammogram
Mammograms are usually performed at outpatient imaging centers or breast centers that are part of a hospital or health system. To schedule a mammogram, call the hospital’s main phone number, scheduling department number, or women’s health or breast center and ask to be connected with someone who can schedule a mammogram.
How quickly a center can get you scheduled for a mammogram depends on the facility and whether you ask for a screening or diagnostic mammogram. If you are concerned that you need to be scheduled sooner than what is offered to you, ask your doctor for assistance.
How to prepare on the day of the mammogram
On the day of the test, it is best not to wear deodorant, antiperspirant, creams, lotions, or perfumes under your arms or on or under your breasts. Sometimes these types of products show up as white spots on x-rays, which could make it harder for the radiologist to read.
If you are premenopausal or perimenopausal, you may want to consider not scheduling a mammogram the week before your period or during your period if possible, because breast tissue can be tender at that time and a mammogram may feel painful.
Otherwise, you do not need to change any normal activities such as exercise, drinking alcohol, or any other parts of your lifestyle before having a mammogram.
What to expect during your mammogram
Before the test, you will be asked to fill out a breast health history questionnaire. You will then be taken to a dressing room to remove your shirt and bra and put on a gown. You will probably need to wait in a waiting room for a few minutes before a technologist takes you to the mammography room.
The technologist will help you remove part of your gown and place each breast, one at a time, on the mammogram machine. Two plates will compress or flatten each breast while a camera attached to the plates takes pictures from different angles. Flattening the tissue gives radiologists — doctors who specialize in using imaging technology to diagnose disease — a better quality image that also uses less radiation than other kinds of x-rays.
It’s normal to be concerned about pain or discomfort while the plates compress your breasts and the camera takes pictures. Some people have some pain, but it usually goes away quickly after the compression, which lasts about 10 to 15 seconds. If you are about to have your period and your breasts are tender, you may have more discomfort than you would at other times of the month. The actual mammogram takes about 10 to 15 minutes.
Paying for your mammogram
Getting the cost of a mammogram covered can be different in different situations, especially if you have a high risk for breast cancer. But there are ways to find help if you have difficulty.
If you are at average risk
Most health insurance companies, under the Affordable Care Act, must cover screening mammograms at no cost for women at average risk who are ages 40 to 50, once a year or once every 2 years.
Many states require Medicaid and public employee health plans to cover screening mammograms. For Medicare beneficiaries aged 40 and older, Medicare pays for yearly screening mammograms and for one baseline mammogram for women ages 35 to 39.
If you are uninsured or underinsured, there are resources to help you get a mammogram at no cost to you. The Centers for Disease Control and Prevention’s National Breast and Cervical Cancer Early Detection Program helps women in each state find programs that will help them get screening and diagnostic mammograms at no cost to them.
People who do not have insurance who pay out of pocket for a mammogram can expect to pay $65 to $380 for a screening mammogram and $150 to $1046 for a diagnostic mammogram.
If you are at high risk
Depending on the laws in your state, if you have a high risk of developing breast cancer, your insurance plan may not cover extra mammogram screenings. If this is your situation, ask your healthcare team for guidance. Sometimes, they can work with your insurance company to help you get coverage or point you to financial assistance resources.
Even if your state does not have laws in place requiring insurance companies to cover high-risk screening, many state legislators have introduced bills to require coverage. There is also a federal bill called the Find it Early Act that was recently introduced to Congress. If passed, the bill would ensure that people at high risk can get the screenings they need at no cost. You can learn more about high-risk coverage laws in your state at DenseBreast-info.org.
If you have concerns about paying for breast cancer screening tests, visit LBBC’s Financial matters section and Financial assistance page.
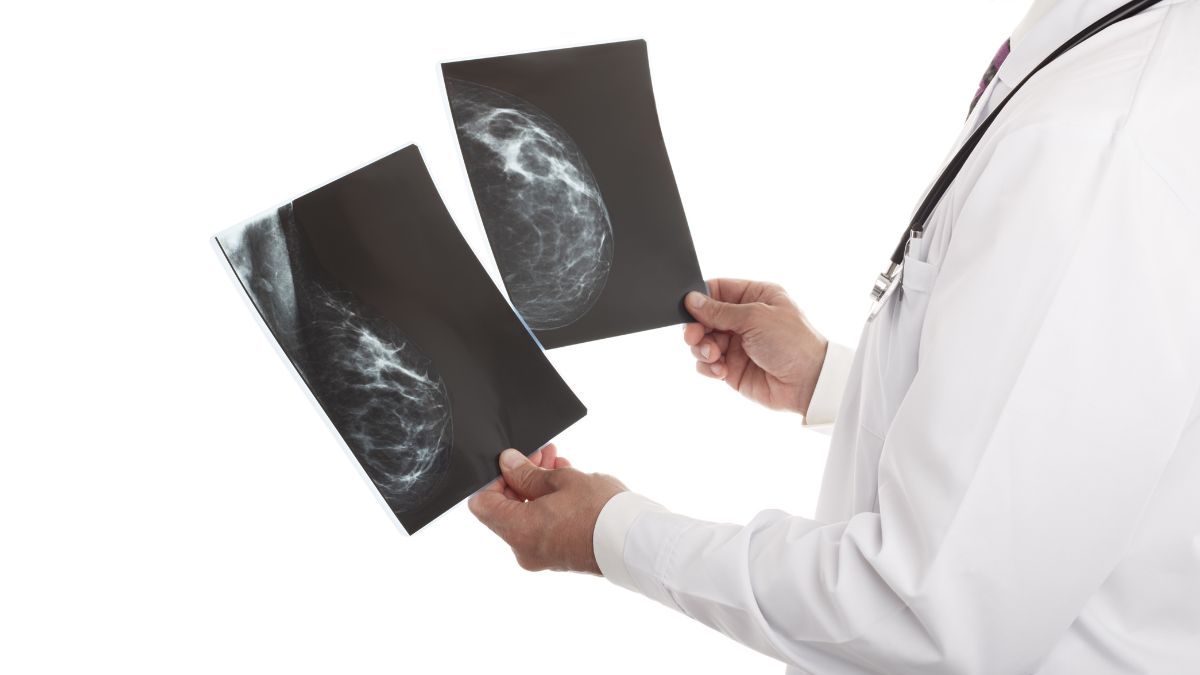
Mammogram results
After a screening mammogram, the speed of receiving results can vary depending on the mammography center. Some centers deliver results before you leave your mammogram appointment. With other centers, you may receive results within 2 to 4 weeks. For a diagnostic mammogram, you can expect to receive your results more quickly. Whether you are having a screening or diagnostic mammogram, you may want to ask the mammography technologist how long you can expect to wait for results.
In some cases, a person may get “called back” for additional imaging after getting a screening mammogram. A recommendation for additional imaging does not mean you have breast cancer. It means the doctors have seen something they want to look at more closely. At LBBC, we know that being called back can trigger fear and anxiety. But most women who get called back for more imaging are not found to have breast cancer.
It’s also important to know that a mammogram alone rarely gives enough information to diagnose breast cancer. If your doctor suspects cancer, you are likely to need other tests to confirm the diagnosis.
How mammogram results are interpreted
A mammogram could find a number of different breast changes, many of which are not cancer. The radiologist will look for:
- Asymmetries that look white on a mammogram
- Areas where breast tissue looks distorted or pulled toward a certain point
- Masses, or areas of abnormal breast tissue, including cysts (non-cancerous, fluid-filled sacs) or fibroadenomas (solid masses that may or may not be cancer)
- Thickening of the skin
- Calcifications (deposits or tiny specks of calcium), which are usually harmless but could be a sign of cancer
- Breast density, a measure of fibrous and glandular tissue as compared to fat tissue in the breast
If your results say you have dense breasts
In some cases, the results report may say that dense breast tissue was found. Dense breasts have more fibrous and glandular tissue than fat tissue. About half of women aged 40 and older have dense breast tissue. Dense breast tissue can make it harder to see cancer because it appears white on a mammogram, and cancer does too. Dense breasts also raise the risk of breast cancer. But talking with your doctor about a high-risk screening plan can help manage that risk.
What to do if you get an abnormal reading
If a radiologist sees one of the findings outlined above or anything that looks abnormal, it doesn’t necessarily mean a cancer diagnosis. The radiologist may recommend additional tests, such as an ultrasound or MRI.
In some cases, the radiologist may also recommend a biopsy. A biopsy is a procedure that removes a sample of tissue. The sample is sent to a lab where a pathologist will examine it under a microscope. If the biopsy results are negative or benign, no cancer was found. If cancer is found, your doctor or nurse will refer you to a breast cancer oncologist or breast surgeon to figure out next steps.
Breast Imaging Reporting and Data System (BI-RADS)
Radiologists use a standard system called Breast Imaging Reporting and Data System (BI-RADS) to describe mammogram findings and results. It uses a numbered system of 0 through 6 that the radiologist who reads your mammogram will use to categorize your results.
Here are the BI-RADS categories:
- BI-RADS 0 means additional testing is needed
- BI-RADS 1 means the result is negative or normal
- BI-RADS 2 means a benign (non-cancerous) finding
- BI-RADS 3 means a probable benign finding and follow-up is suggested
- BI-RADS 4 means there is a suspicious abnormality and biopsy should be considered
- BI-RADS 5 means the finding is highly suggestive of cancer and biopsy is strongly recommended
- BI-RADS 6 means that the biopsy has confirmed cancer; this BI-RADS category is used with mammogram or other diagnostic imaging that is performed after a biopsy
Mammogram accuracy
Mammograms are the best breast cancer screening tests available, but they are not 100% accurate in diagnosing breast cancer. They miss 1 in 8 breast cancers. If you are concerned about the accuracy of your mammogram, talk with your healthcare team about your individual risk of breast cancer and whether they may recommend additional imaging techniques.
Mammogram risks
While mammograms expose the breasts to a small amount of radiation, the benefits of early detection outweigh the risks of radiation exposure.
Mammogram FAQs
Here are answers to some of the most common questions about mammograms.
Do mammograms hurt?
You may have brief discomfort or pain during the 10 to 15 seconds when your breast is compressed between the machine’s plates, especially if you get the test right before or during your period.
How often should I get a mammogram?
Most professional organizations recommend getting a screening mammogram every year. Some groups recommend getting a screening mammogram every other year. Talk with your doctor about what is the best choice for you.
At what age should I start getting mammograms?
If you are at average risk for breast cancer, most professional organizations recommend you start getting a screening mammogram at age 40. If you are at high risk, some organizations recommend you start at age 25 or 35. It’s best to talk to your doctor about what age is right for you, depending on your risk factors.
Does a mammogram show under my armpit?
While mammograms may be able to see some parts of your underarm, they may not always be able to view all of it. Breast cancer cells can sometimes spread to lymph nodes — small immune system organs — in the armpit area. The most accurate way to tell if cancer is in lymph nodes is through sentinel lymph node biopsy or axillary lymph node dissection surgery. You can learn more on the lymph node surgery page.
Do mammograms have negative side effects?
Mammograms expose the breasts to very small amounts of radiation, but the benefits of getting a mammogram outweigh any harm.
Related news
- Breast cancer is personal: Your treatment should be, too | SABCS 2025
- Paging chat: AI tools offer progress and opportunity in breast cancer | ASCO 2025
- New breast cancer drug camizestrant shows better outcomes with early ESR1 detection | ASCO 2025
- Personalized medicine in MBC: What it means for you
Related downloads
View allStay connected
Sign up to receive emotional support, medical insight, personal stories, and more, delivered to your inbox weekly.
Reviewed and updated: August 28, 2023
Reviewed by: Kristin Brill, MD, FACS
Tagged:

Living Beyond Breast Cancer is a national nonprofit organization that seeks to create a world that understands there is more than one way to have breast cancer. To fulfill its mission of providing trusted information and a community of support to those impacted by the disease, Living Beyond Breast Cancer offers on-demand emotional, practical, and evidence-based content. For over 30 years, the organization has remained committed to creating a culture of acceptance — where sharing the diversity of the lived experience of breast cancer fosters self-advocacy and hope. For more information, learn more about our programs and services.
